Have you ever heard of snapping scapula syndrome? If you answered no, I would not be too surprised. Whilst this condition is more common than you may think, it seems to be underappreciated within the physiotherapy. Thus, this article will discuss snapping scapula syndrome including what it is, why it occurs and what you need to do to fix it!
As a sports physiotherapist, it is important that you not only rehabilitate athletes but ensure that they are fully fit to return to play. As many of you are fully aware, objective measures such us a full active range of motion does not determine an athlete’s readiness to RTP. Accordingly, a comprehensive assessment of an athlete’s function, via functional performance testing, becomes an absolute assessment necessity. This article will discuss current research on the the role and implementation of functional performance testing, as well as some tests that you may use in your own clinical practice.
Now, we have discussed Arnold Schwarzenegger on this site before, in a post about the psychology of sports injury and physiotherapy. However, it seems that man was quite the insightful gentleman. In his text The Encyclopedia of Modern Bodybuilding Arnold discusses the mind to muscle connection and the importance of not just lifting a weight up and down, but having your “mind in the muscle”. This article will discuss new research into conscious correction of scapular position.
Those in the world of sports physiotherapy would be aware of the frequency with which we encounter episodes of patellar instability. Whilst much research is performed in the adult population, it is important to recognise patellar dislocation as one of the most common acute knee injuries in children. Accordingly, this article will discuss new research into the predictors of patellofemoral joint instability in the adolescent and paediatric populations.
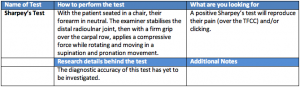
Introduction Sports physiotherapists regularly assess and treat shoulder pathologies. In my clinical practice, shoulders would place in the top 3 most common conditions (along with back and knee presentations). Given the frequency with which we see these problems, there is much interest in the best assessment and rehabilitation techniques for shoulder problems. This article will […]
Many of the world’s sports physical therapists and physiotherapists spend their weekends at sporting events around the world. Unfortunately, many of us do not have the support of a huge medical team around us, such as that available to James Sutherland at Wallabies games. Therefore, we are often the most highly trained “medical” staff at any given event, and when it comes to injured athletes the buck stops with us. This means we require knowledge on a variety of conditions that may not be “sports” injuries and many abdominal injuries may fall outside the expertise of a physio.
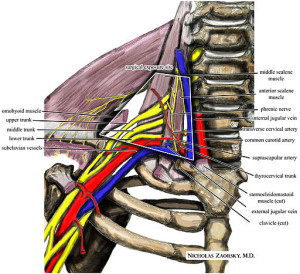
Introduction The condition discussed in this article, you will come to find, is quite complex and can be a battle for the physiotherapist and physical therapist. Thoracic outlet syndrome is considered to be a collection of quite diverse syndromes rather than a single entity (Yanaka et al., 2004), and therefore, accurate diagnosis and enlightened treatment […]
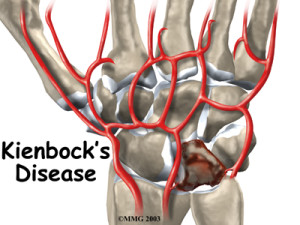
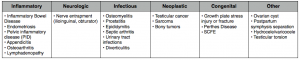
Kienbock’s Disease is a rare and infrequently discussed source of wrist pain that you could definitely encounter in your clinical practice. The condition is named after the Viennese radiologist Robert Kienbock who presented his findings on the disorder in his 1910 publication ‘Concerning traumatic malacia of the lunate and its consequences’. This condition, discussed in depth below, primarily affects people between 15 and 40 years old and has been documented in athletes from many sports that include repetitive use of the wrist e.g. golf, tennis, martial arts, etc . Therefore, if you work with athletes from these sports, you should remain on high alert for the occurrence of Kienbock’s disease.
Introduction With a name like that, all physiotherapists will remember this one! But how much detail is remembered? Have a quick think about how many wrist patients you see, compared to knee or back patients. If you are in a private practice/outpatient clinic with a demographic anything like mine you will be seeing mostly backs, […]
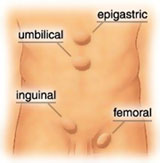
Groin pain is a common complaint in sports involving running, kicking and explosive changes of direction, and as such is frequently encountered by the sports physiotherapist. In soccer, groin and lower abdominal pain accounts for 10-13% of injuries per year. However, due to the number of potential differential diagnoses for athletes with chronic pain in the groin and lower abdominal region only a small proportion of athletes are eventually diagnosed with athletic pubalgia (sports hernias). Athletic pubalgia is a poorly understood disease process and it is imperative that athletes with the condition are managed appropriately as the symptoms can eventually limit the athlete’s participation in training and playing.
In the past this site has featured some lighter, colloquial blog posts. These articles discuss issues related to the greater physiotherapy community. Thus, I present a few mantras I have heard, adapted or made up for the physios to live by in the coming year.
Radial tunnel syndrome is rare, it is challenging to differentially diagnose and can be a monster to manage. If you have a recalcitrant case of tennis elbow then this post will interest you! This article discusses the best available evidence for assessment and management of radial tunnel syndrome.