Introduction
Ankle injuries are a ridiculously common sports injury. Fong et al (2007) found that ankle injuries are the most common injuries in a wide variety of popular sports. It has been suggested that syndesmosis injuries account for about 11% of these ankle injuries (Williams & Allen, 2010; Mulligan, 2011). Furthermore, ankle syndesmosis injuries (or “high” ankle sprains) have high occurences during athletic activities, particularly those that involve twisting or cutting activities (think Benji Marshall / Brandon Lloyd / Ronaldo : to cover most countries!)
This means that you sports physiotherapists will regularly see these injuries. It is very important that you are aware of EBP for this condition.
Anatomy
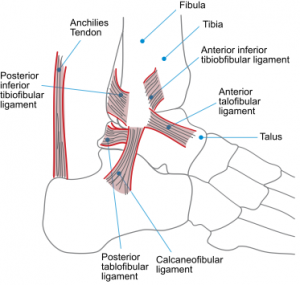
Whilst I won’t labour the anatomy (you guys would all know it anyway….wouldn’t you?). However, I just wish to discuss the contributions of the ligamentous restraints of the distal tibiofibular joint (Ogilvie-Harris et al., 1994):
- Anterior Inferior Tibio-fibular Ligament: Provides ~ 35% of the restraint. Travels inferiorly in a medial to lateral direction.
- Posterior Inferior Tibio-fibular Ligament: Provides ~ 40% of the restraint. Stronger and thicker than the AITFL.
- Interosseous Membrane: Provides the remaining ~ 25% of the restraint.
Biomechanics
Again, the biomechanics are most likely well understood, I think it is important that I confirm one point. The inferior or distal tibio-fibular joint is a fibrous syndesmotic joint. It spreads to accommodate the trapezoidal talus (which is 3-4mm larger anteriorly than posteriorly) during dorsiflexion.
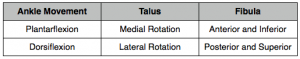
The following table displays the concurrent movements of the ankle, talus and fibula:
Mechanism Of Injury
Given our re-found understanding of the anatomy and the biomechanics, we can the discuss the mechanisms of injury for injury to the distal tibio-fibular joint or syndesmosis. The syndesmotic ligaments are challenged by excessive foot external rotation in ankle dorsiflexion.
There are two main cited mechanisms for ankle syndesmosis injuries (Norkus & Floyd, 2001):
- ER of Foot on Tibia
- Hyper-dorsiflexion of the Ankle
Assessment and Diagnosis of Ankle Syndesmosis Injuries
The assessment and diagnosis of ankle syndesmosis injuries is one that requires careful integration of subjective, objective and radiographic information. Your assessment should not only diagnose but identify those who require surgery and exclude other differential diagnoses.
Subjective Examination
Athlete will often report:
- Mechanism: similar to that reported above
- Pain: anterolateral ankle pain, however, frequently “higher” than that of a lateral ankle sprain
Objective Examination
- Observation: swelling seen proximal to ankle joint axis. Less prone to swelling than lateral ankle sprains given that the ligaments are extra-capsular (Fites et al., 2006).
- AROM: typically painful both saggital plane movements
- Palpation: tender on palpation of AITFL and PITFL (differentiate from lateral ligament complex). AITFL tenderness has a positive predictive value of 70% (Alonso et al., 1998). It has been noted that tenderness proximally along the interosseous membrane is indicative of more severe injury.
- Ottowa Ankle Rules: required to exclude possibility of a fracture.
- Ligament Testing: to exclude concomitant ligament injuries.
- Special Tests: the following special tests search for pain reproduction (not ligament laxity). The diagnostic accuracy of any is not well established.
Squeeze Test
Kleiger’s Test (DF/ER Stress Test)
Dorsiflexion Compression Test
Imaging
X-Ray: radiological examination should include:
- AP
- Lateral
- Mortise
- Bilateral weight-bearing views
The diagnostic accuracy of x-rays has been questioned, showing poor sensitivity. False negative rates have been reportedly as high as 58% (Takao et al., 2003).
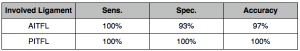
MRI: Has shown much greater diagnostic accuracy for identification of ligamentous injury. See table below:
Surgical Management
Surgical management is indicated in the following cases (Williams & Allen, 2010; Mulligan, 2011):
- Frank Instability on Radiographs
- Presence of # requiring fixation
- Other surgically treatable pathologies (repairable syndesmotic ligament tear, latent instability, scarring or calcification of the syndesmosis)
In most other cases conservative management is indicated.
Conservative Management
There are no hard and fast rules on rehabilitation time-frames. When conservatively managing ankle syndesmotic injuries progression of therapy is governed by symptomatic response (Mulligan, 2011). The conservative rehabilitation can be thought about in 3 phases:
Acute Phase
Aims: Protection of healing tissues and control the initial inflammatory response.
- PRICE
- Protection: taping or boot
- Soft Tissue Massage (and effleurage for swelling)
- Manual Therapies: low grade talocrural, subtalar and tibio-fibular mobilisations
- Cross-Training
Sub-acute Phase
Aims: Regain ROM, strength and neuromuscular control
- Contrast thermal therapies
- AROM exercises
- PROM/PWB Stretches
- Gastrocnemius and other peri-articular ankle strengthening (e.g. 4 way thera-band)
- Don’t ignore proximal muscles e.g. hip
- Manual Therapies: higher grade mobilisations
- Progress to plyometric training
- Proprioceptive and neuromuscular exercises
Sport-Specific Phase
- Increasing complexity of drills and training
- Agility skills
- High level balance training
- Plyometric drills
- Gradual and progressive return to team training
RTP Considerations
Again, there are no hard and fast return to play rules. However, widespread clinical experience is that AITFL or “high” ankle sprains have a longer recovery and rehabilitation period than lateral ankle sprains (Williams & Allen, 2010). As an overgeneralised rule; syndesmotic ankle sprains typically take 6 – 8 weeks to recover. Individually, Mulligan (2011) suggests that return to play decisions should be made through:
- Functional Tests: see here.
- Training Tolerances
- Objective Outcome Measures: such as the Foot and Ankle Disability Index
What are your thoughts on the management of syndesmotic ankle sprains. Be sure to let me know in the comments or catch me on Facebook or Twitter
If you require any sports physiotherapy products be sure check out PhysioSupplies (AUS) or MedEx Supply (Worldwide)
Photo Credit: Dplanet
References
Alonso, A., Khoury, L., & Adams, R. (1998). Clinical tests for ankle syndesmosis injury: reliability and prediction of return to function. Journal of Orthopaedicand Sports Physical Therapy, 27, 276-284.
Dattani, R., Patnaik, S., Kantak, A., Srikanth, B., & Selvan, T. P. (2008). Injuries to the tibiofibular syndesmosis. Journal of Bone and Joint Surgery British., 90, 405-410.
Fites, B., Kunes, J., Madaleno, J., & Johnson, D. L. (2006). Latent syndesmosis injuries in athletes. Orthopedics, 29, 124-127.
Fong DT, Hong Y, Chan LK, Yung PS, Chan KM. A systematic review on ankle injury and ankle sprain in sports. Sports Med. 2007;37(1):73-94
Norkus, S. A., & Floyd, R. T. (2001). The anatomy and mechanism of syndesmotic sprains. Journal of Athletic Training., 36, 68-73
Ogilvie-Harris, D. J., Reed, S. C., & Hedman, T. P. (1994). Disruption of the ankle syndesmosis: biomechanical study of the ligamentous restraints. Arthroscopy,10, 558-560.
Takao, M., Ochi, M., Oae, K., Naito, K., & Uchio, Y. (2003). Diagnosis of a tear of the tibiofibular syndesmosis: the role of arthroscopy of the ankle. Journal of Bone and Joint Surgery., 85B, 324-329.
Mulligan EP. Evaluation and management of ankle syndesmosis injuries. Physical Therapy in Sport 12 (2011) 57-69
Oae K, Takao M, Naito K, Uchio Y, Kono T, Ishida J, Ochi M. Injury of the Tibiofibular Syndesmosis: Value of MR Imaging for Diagnosis. Radiology 2003;227, 155-161.
Williams GN, Allen EJ. Rehabilitation of Syndesmotic (High) Ankle Sprains. Sports Health: A Multidisciplinary Approach 2010 2: 460
Related Posts
Trackbacks








[…] Ankle Syndesmosis Injuries: Evidence Based Diagnosis and …May 6, 2011 … It has been suggested that syndesmosis injuries account for about 11% of these ankle injuries (Williams & Allen, 2010; Mulligan, 2011). […]