Introduction
Ankle injuries are a ridiculously common sports injury. Fong et al (2007) found that ankle injuries are the most common injuries in a wide variety of popular sports. In fact, it has been suggested that ankle injuries account for 10-30% of all sports injuries; 77% of which are lateral ankle sprains (Fong et al., 2007). Thus, it goes without saying that knowledge of evidence based management and current best practice is essential for lateral ankle sprains. This article will discuss the current evidence for the use of bracing following acute ankle sprains.
Lateral Ankle Anatomy
Whilst I never labour the anatomy (you guys would all know it anyway….wouldn’t you?), I will discuss it quickly. As you well know there are both static and dynamic contributors to limit excessive ankle inversion, these are discussed below.
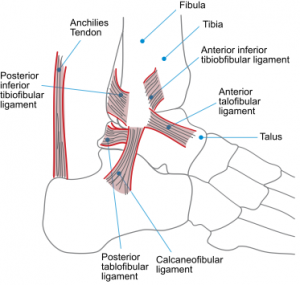
Static Stabilisers (collectively known as the lateral ligamentous complex) are (Safran et al., 1999):
- Anterior Talofibular Ligament (ATFL): an intracapsular structure (10-12mm x 2-5mm) arises from the anterolateral malleolus and inserts onto the neck of the talus.The weakest of the lateral ligaments it is the primary stabiliser during ankle inversion and plantarflexion (think ballet dancers) and is thus most commonly injured in this position.
- Calcaneofibular Ligament (CFL): extracapsular structure (6mm thick) it arises from the lateral malleolus and fans at 10-40° to insert onto the lateral side of the calcaneus.
- Posterior Talofibular Ligament (PTFL): the strongest of the 3 arising from the digital fossa of fibula and inserting onto the lateral tubercle of the posterior talus. Rarely injured secondary to its tautness only in end-range dorsiflexion.
Dynamic Stabilisers:
- Provided by the peroneus longus and peroneus brevis muscles
- The strength of the peroneus longus and brevis tendons has been shown to be greater than the ATFL and approximately equal to the CFL (Safran et al., 1999)
To Brace Or Not To Brace?
Many sports physiotherapists would know the challenge that lateral ankle sprains can provide. Acutely, most will follow the PRICE principles; Protection, Rest, Ice, Compression, Elevation. Ideally, functional treatment will be used for lateral ankle sprains, as this has been shown to provide superior outcomes (Kannus & Renstrom, 1991; Jones & Amendola, 2007). However, when utilising the “protection” principle that is necessary to protect the healing ligaments from further injury it is often challenging to make clinical decisions on the most appropriate clinical technique. As previously suggested, below we will discuss the current evidence for the use of bracing following acute ankle sprains.
Outcomes For Brace vs. No Brace
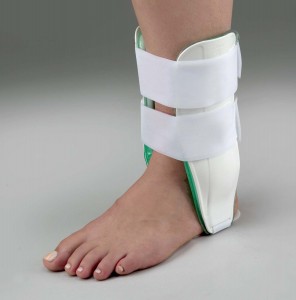
Kemler et al. (2011) performed a systematic review of the literature comparing the outcomes of either bracing or using no brace following acute ankle sprains. “Brace” was a broad term, but most commonly utilised was an Aircast type brace. This was compared with other forms of protection including TubiGrip and elastic support bandage (and quite rarely supportive taping). The systematic review included 8 studies, 7 of which scored well on the Pedro Score and were deemed ‘high quality’. Unfortunately, due to the heterogeneity of studies the authors of the study were unable to pool the results. A brief summary of their findings is presented below.
Recurrent Sprains or Instability
One of the biggest challenges is injury recurrence or re-sprain, which has been reported as 3 – 34% (van Rijn et al., 2008). Subsequently, there is the potential for chronic ankle instability which can lead to early onset osteoarthritis (Harrington, 1979). 4 studies evaluated injury recurrence and their follow-up periods varied between 5 weeks and 2.8 years. 2 studies evaluated ongoing instability. Overall, there was no significant difference between groups for re-injury or instability (Kemler et al., 2011).
Pain and Swelling
We are all aware of the pain that athletes suffer following ankle sprain. The authors found no differences for the pain (V.A.S, time to pain free running) or swelling related outcomes between “braced” and “non-braced” groups.
Functional Outcomes
Now, this was interesting. 5 of the included studies evaluated functional outcomes. These included the Foot and Ankle Outcome Score (FAOS) and Karlsson Scoring Scale. 2 of the 3 studies that evaluated shorter term outcomes, that is Lamb et al. (2009) and Boyce et al. (2005) found strong evidence of the benefit of bracing over compression with Tubigrip/elastic bandage at 12 and 4 weeks respectively. However, when you look at the longer term picture, as did Beynonn et al. (2006) and Karlsson et al. (1996), 6 and 12-24 months respectively, there was no clear benefit of bracing over non-bracing.
So this seems to suggest that there is a positive effect of bracing over non-bracing i.e. with tubigrip or an elastic support bandage (Kemler et al., 2011). What would be very interesting would be a direct comparison between bracing and supportive taping, conceivably the differences in short-term outcomes may not be so significant.
Return to Play, Work or Daily Activities
Whilst there was a positive trend, the included studies found no significant differences in terms of return to play, daily activity or work outcomes (Kemler et al., 2011)
Limitations of This Research
As has been suggested throughout the article there are some limitations to this research. This is significant heterogeneity in the studies including types of bracing, differences of control measures (bandage, Tubigrip), and varying populations i.e. both athletic and non-athletic populations. Furthermore, in most included studies there was no active treatment (i.e. physiotherapy/physical therapy) undertaken by the participants. Thus, it is challenging from the current available evidence to make definite decisions regarding bracing following acute ankle sprain, and clinical conclusions made from this research should be made with caution.
What Are Your Thoughts?
What are your experiences with ankle bracing? Do you brace your athletes following acute ankle sprain? Tape? Tubigrip? I would love you to let me know in the comments or catch me on Facebook or Twitter.
References
Beynonn BD, Rentrom PA, Haugh L, et al. A prospective, randomized clinical investigation of the treatment of first-time ankle sprains. Am J Sports MEd 2006;34(9):1401-12.
Boyce SH, Quigley MA, Campbell S. Management of ankle sprains: a randomised controlled trial of the treatment of inversion injuries using an elastic support bandage or an Aircast ankle brace. Br J Sports Med 2005;39(2):91-6
Fong DT, Hong Y, Chan LK, Yung PS, Chan KM. A systematic review on ankle injury and ankle sprain in sports. Sports Med. 2007;37(1):73-94
Harrington KD. Degenerative arthritis of the ankle secondary to long-standing lateral ligament instability. J Bone Joint Surg Am 1979;62(3):354-61
Jones MH, Amendola AS. Acute treatment of inversion ankle sprains immobilization versus functional treatment. Clin Orthop Relat Res 2007;455:169-172
Kannus PM, Renstrom P. Treatment for acute tears of the lateral ligaments of the ankle: operation, cast or early controlled mobilization. J Bone Joint Surg Am 1991;73:305-12.
Karlsson J, Eriksson BI, Sward L. Early functional treatment for acute ligament injuries of the ankle joint. Scand J Med Sci Sports 1996;6:341-5
Lamb SE, Marsh JL, Hutton JL, et al. Collaborative Ankle Support Trial (CAST Group). Mechanical supports for ankle, serve ankle sprain: a pragmatic, multicentre, randomised controlled trial. Lancet 2009;373(9663):575-81.
Ogilvie-Harris, D. J., Reed, S. C., & Hedman, T. P. (1994). Disruption of the ankle syndesmosis: biomechanical study of the ligamentous restraints. Arthroscopy,10, 558-560.
Safran MR, Benefetti RS, Bartolozzi AR, Mandelbaum BR. Lateral ankle sprains: a comprehensive review. Part 1: etiology, pathoanatomy, histopathogenesis, and diagnosis. Med. Sci. Sports Exerc 1999;31(7):429-S437
van Rijn RM, van Os AG, Bernsen RM, et al. What is the clinical course of acute ankle sprains? A systematic literature review. Am J Med 2008;121(4):324-31
Related Posts