Introduction
Sports physiotherapists regularly assess and rehabilitate shoulder dysfunctions and pathologies. As a sports physiotherapists it is important to evaluate the contributing factors to shoulder pathology. A common contributor, seen in 68-100% of shoulder injuries, is scapular dyskinesis. Accurate and comprehensive assessment of scapular dyskinesis is essential to identify alterations in normal scapulo-humeral rhythm. If you treat shoulders, ‘treating the scapula’ is absolutely paramount … ignore it at your own peril.
What Is Scapular Dyskinesis?
Quite simply the term ‘Scapular dyskinesis’ is a collective term that refers to dysfunctional movement of the scapula i.e. ‘dys’—alteration of , ‘kinesis’— movement (Kibler & Sciascia, 2010). It has been shown that scapular dyskinesis is a non-specific response to a painful condition in the shoulder i.e. it is not a response to any specific pathology. It has many causative factors, which may include:
- Muscle weakness
- Muscle imbalance, including
- Altered muscle activation patterns
- Nerve injury
- Muscle Injury
- Osteo-ligamentous injury
- Proprioceptive dysfunction
In What Conditions Do We See Scapular Dyskinesis?
It has been suggested that scapular dyskinesis is present in 68-100% of shoulder injuries (Kibler et al., 2003). One of the 3 types of scapular dyskinesis (discussed below) are commonly seen in (Kibler & Sciascia, 2010):
- Impingement: the scapular dyskinesis present in impingement patients regularly displays reduced acromial upward rotation and winging (which is increased scapular internal rotation and anterior tilt )(Ludewig and Cook, 2000).
- Rotator Cuff Injury
- M.D.I: frequently display altered scapulo-humeral rhythm and rotator cuff activation patterns (Ogston and Ludewig, 2007, Illyés and Kiss, 2006).
- Labral Injury: altered scapular positioning and motion increases stress on the anterior shoulder, and can increase the ‘peel-back’ load on the labrum (Burkhart et al., 2003).
- Traumatic Injuries: clavicular fractures, AC joint injuries.
Types of Scapular Dyskinesis
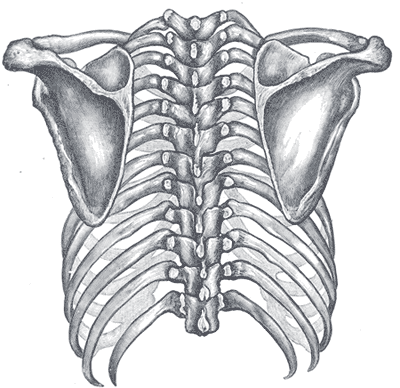
Type 1: Inferior Angle Prominence
- At Rest: the inferior medial scapular border may be prominent dorsally.
- Abnormal Motion: inferior angle tilts dorsally and the acromion tilts ventrally over the top of the thorax. The axis of the rotation is in the horizontal plane.
- Common Associated Findings: Tightness/shortening of pectoralis minor (Borstad & Ludewig, 2005)
Type 2: Medial Border Prominence
- At Rest: medial border is prominent dorsally
- Abnormal Motion: medial border of scapula tilts dorsally of the thorax. Rotation axis is in the frontal plane
- Common Associated Findings: weakness/reduced activation serratus anterior and lower traps.
Type 3: Superior Border Prominence
- At Rest: Superior border generally elevated, scapula often anteriorly displaced
- Abnormal Motion: shoulder shrug motion evident. Axis of motion in the saggital plane.
- Common Associated Findings: Tightness/overactive upper trapezius, weakness/reduced activation lower trapezius.
Assessment of Scapular Dyskinesis
The assessment of potential scapular dyskinesis should be undertaken with a few goals in mind. Think… what am I looking for and what I am I going to do with this information? Well, you are looking to:
- See if there is an altered scapular resting position
- See if scapular dyskinesis is present or absent (more later)
- Identify potential causes (think proximally AND distally)
- Assess the impact of scapular dyskinesis on symptoms through special testing
Visual Observation
You should undertake a thorough evaluation of the patient’s scapulo-humeral rhythm. Components of the examination will include both static and dynamic evaluation, possibly under loaded and unloaded circumstances.
Posterior Observation; includes, but is certainly not limited too, evaluation of:
- Spinal Posture
- Resting scapular position: side-to-side asymmetry
- Inferior medial border (?Type 1)
- Medial border prominence (?Type 2)
- Superior border prominence (?Type 3)
Lateral Observation; includes, but again is certainly not limited too, evaluation of:
- Spinal Posture
- Protraction/Retraction
- Humeral head position
- Presence of dyskinetic patterns as above
Corrective Manoeuvres/Special Testing
Scapular Assistance Test
This test is employed if you have identified the presence of scapular dyskinesis in your above testing procedures. You will apply gentle pressure assisting scapular upward rotation as the patient elevates their arm (see video below). A positive result is a reduction in the patient’s symptoms or improvement in ROM, and suggests the use of scapular training in the rehabilitation of the patient.
Scapular Retraction Test
This test compares either the strength of supraspinatus or results of dynamic labral shear test in the patients normal position, and then with the scapula retracted (see video below). Positive result is when strength is improved or labral symptoms are reduced in retraction. This works on the theory that the scapular is the cornerstone of shoulder motion. It is necessary for the scapular to be stabilised in relative retraction to maximise activation of the rotator cuff musculature (Kibler and Sciascia, 2006; Smith et al., 2006).
Evaluation of Contributors/Causative Factors
As previously suggested, it is not enough to identify that scapular dyskinesis is present. It is also necessary to objectively assess the potential contributing/causative factors, including (as a start);
- Passive Scapular Mobility
- Lower Trapezius MMT/function
- Serratus Anterior MMT/function
- Pectoralis Minor muscle length and palpation (tautness/TrPs)
- Upper Trapezius/Levator Scapulae muscle length (tautness/TrPs)
- Glenohumeral ROM (including posterior shoulder mobility and Glenohumeral Internal Rotation Deficit)
- Cervical and Thoracic ROM
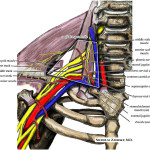
- Potential Neural examination including long thoracic nerve assessment (Bertelli and Ghizoni, 2005).
A Word About Relialidity (Yep, Reliability and Validity In One)
McClure et al. (2009) and Tate et al. (2009) investigated the reliability and validity of a clinical method for identifying scapular dyskinesis. They delivered some interesting results. They found moderate inter-rater reliability (average κ = 0.57) for classifying the scapular motion as normal, subtle dyskinesis or obvious dyskinesis i.e. not Type 1 – 4 (McClure et al., 2009). This compares favourably to the inter-rater reliability (average κ = 0.42) displayed by Kibler et al. (2002) who attempted to distinguish between the sub-types of dyskinesia. Tate et al. (2009) evaluated the validity of the method for assessing scapular dyskinesis. Whilst there was notable differences in scapular motion in those classified as normal and obvious dyskinesis, this was not related to shoulder symptoms in that population (overhead athletes).
Take Home Messages
- Scapular dyskinesis is evident in many shoulder pathologies
- Look carefully: from the front, side, back, dynamic, static, loaded and unloaded!
- Comprehensive assessment of scapular dyskinesis requires evaluation of potential contributing/causative factors
- Remember the reliability and validity. Ask the question: Is this abnormal, relevant and fixable?
- For some info on treatment of scapular dyskinesis; some great info here.
What Are Your Thoughts?
I would love to know what your thoughts and experiences are when dealing with assessment of scapular dyskinesis. be sure to let me know in the comments or catch me on Facebook or Twitter
If you require any sports physiotherapy products be sure check out PhysioSupplies (AUS) or MedEx Supply (Worldwide)
Stay Tuned: Our next post will discuss Treatment for Scapular Dyskinesis.
References
Bertelli JA, Ghizoni MF. Long Thoracic Nerve: Anatomy and Functional Assessment. The Journal of Bone & Joint Surgery. 2005; 87:993-998
Borstad JD, Ludewig PM. The effect of long versus short pectoralis minor resting length on scpaular kinematics in healthy individuals. J Orthop Sports Phys Ther 2005;35(4):227-38.
Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part I: pathoanatomy and biomechanics. Arthroscopy 2003;19:404–20.
Illyés A, Kiss RM. Kinematic and muscle activity characteristics of multidirectional shoulder joint instability during elevation. Knee Surg Sports Traumatol Arthrosc 2006;14:673–85.
Kibler WB, Uhl TL, Madduz JW, Brooks PV, Zeller B, McMullen J. Qualitative clinical evaluation of scapular dysfunction: a reliability study. J Shoulder Elbow Surg. 2002;11(6):550-556.
Kibler WB, McMullen J: Scapular dyskinesis and its relation to shoulder pain. J Am Acad Orthop Surg. 2003;11:142-151.
Kibler WB, Sciascia A, Dome D. Evaluation of apparent and absolute supraspinatus strength in patients with shoulder injury using the scapular retraction test. Am J Sports Med 2006;34:1643–7.
Kibler WB, Sciascia A. Current concepts: scapular dyskinesis. Br J Sports Med 2010;44:300–305.
Ludewig PM, Cook TM. Alterations in shoulder kinematics and associated muscle activity in people with symptoms of shoulder impingement. Phys Ther 2000;80:276–91.
McClure P, Tate RA, Kareha S, Irwin D, Zlupko E. A clinical method for identifying scapular dyskinesis, part 1: reliability. Journal of Athletic Training 2009;44(2):160-164.
Myers JB, Laudner KG, Pasquale MR, et al. Scapular position and orientation in throwing athletes. Am J Sports Med 2005;33:263–71.
Ogston JB, Ludewig PM. Differences in 3-dimensional shoulder kinematics between persons with multidirectional instability and asymptomatic controls. Am J Sports Med 2007;35:1361–70.
Smith J, Dietrich CT, Kotajarvi BR, et al. The effect of scapular protraction on isometric shoulder rotation strength in normal subjects. J Shoulder Elbow Surg 2006;15:339–43.
Tate RA, McClure P, Kareha S, Irwin D, Zlupko E. A clinical method for identifying scapular dyskinesis, part 2: validity . Journal of Athletic Training 2009;44(2):165-173
Related Posts
Comments








A lot is always said about an under-active Lower Traps and over active Upper Traps as a contributor to shoulder dysfunction. What about an under-active Upper Traps with a resultant depressed and downwardly rotated scapula. I reckon this is a far more common presentation in not only athletes, but also the general population who have shoulder dysfunction, both G/H instability and impingement syndromes.
I often see patients who present this way and have been given lower traps drills as their rehab program, and not surprisingly have not been improving. Clearly if a shoulder is depressed and downwardly rotated, then trying to lower it further with low traps setting will only serve to propagate/worsen the situation?
Keep an eye out for a similar scapula presentation in your patients with chronic Cx pain and headaches too..
and if all this makes you more confused then do yourself a favour and do a Lynn Watson course!
Great website by the way…
cheers
Loved the testing protocol. Good info here, thanks for putting it all together
Great post, I have been reading your post since the first pod cast. I recommend this site to my undergraduates.
Keep up the good work
Thanks Rob! Love your support!
thanks for giving me this kind of valuable materials and treatment videos.
From presentations i have seen I have that a common problem in g/h dysfunction is an overactive Lev Scap and not overactive upper traps, motor control exercises of upper traps and STM to lev scap have reduced symptoms ! i was wondering has any other clinicians found this?
I’ve been struggling with some sort of scapular dyskinesis for awhile. If I sent you a video of me going through these motions would you be able to take a look and diagnose?
Hi Eric,
Yes I would – but I would not necessarily be able to make clear judgements on the best treatments. My best advice – chase up a good shoulder physio in your local area.