Introduction
With a name like that, all physiotherapists will remember this one! But how much detail is remembered? Have a quick think about how many wrist patients you see, compared to knee or back patients. If you are in a private practice/outpatient clinic with a demographic anything like mine you will be seeing mostly backs, knees, shoulders, ankles – but not so many wrist presentations. Regardless of the number of wrist injuries you see in a typical week your patients will still be expecting the same high level of accuracy and efficiency you offer with other regions of the body.
With Brukner and Khan’s latest edition of the Clinical Sports Medicine (2011) listing TFCC tears amongst 11 other subacute/chronic conditions (with pain on the ulnar aspect of the wrist) and at least 9 acute conditions we really need to have our diagnostician hats firmly pulled on when dealing with wrist patients.
Background Information and Anatomy
The structure of interest has been referred to as the Triangular FibroCartilage Complex since 1981 when Palmer and Werner first introduced it (Palmer & Werner, 1981). Anatomy is one of the fundamental knowledge bases of a good diagnosis, so I am sure you will allow me to describe the relevant anatomy.
The TFCC is comprised of:
- Triangular Fibrocartilaginous disc – also called an ‘Articular disc’
- Volar (palmar) and dorsal radio-ulnar ligaments
- The meniscus homologue (or homolog)
- The homologue is the connective tissue between the disc and the triquetrum
- Ulnar collateral and ulno-carpal ligaments
- Sheath of the extensor carpi ulnaris
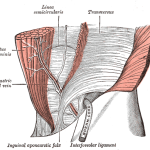
The TFCC binds the distal ends of the ulna and radius together by its attachment to the medial edge of the ulnar notch of the radius it extends transversely, like a hammock, between the two bones. Its apex is then attached to the lateral side of the base of the styloid process of the ulna. This allows the proximal surface of the triangular disc to articulate with the distal aspect of the head of the ulna. Approximately the central 80% of the TFCC is considered to be avascular, limiting the healing potential of tears in this area.
What Does The TFCC Do?
The TFCC is considered to perform the following roles:
- Stabilise the ulno-carpal and distal radio-ulnar joints
- Transmit and distribute load from the carpus to the ulna
- Carries about 20% of the axial load from wrist to forearm
- Permits complex movements of the wrist (Nakamura, Yabe, & Horiuchi, 1996)
Mechanism of Injury
Wrist injuries are often complex and their management will vary greatly; as such it is vital that the correct diagnosis is made. If you look specifically at the athletic population TFCC tears are more frequently seen in gymnastics, hockey, racquet/batting sports, boxing, and pole vaulting. This is due to the repetitive high forces on the wrist that will often be in extension or ulnar deviation, or both (Parmelee-Peters & Eathorne, 2005). These injuries can also occur from falls with an outstretched hand and in the manual working population. The injury will often occur whilst the wrist is bearing weight.
Mikic (1978) demonstrated the age related changes in the TFCC. He dissected 180 wrist joints from 100 fresh cadavers aged between that of a foetus to 94 years old. His findings were that the TFCC sustained significant age/use related degeneration and that these changes always occurred centrally, again suggesting poor healing capabilities. His research also showed that as of the fifth decade there were no TFCC’s with ‘normal appearance’ and that over 50% of 60+ year olds had degeneration with disc perforation.
In the below table you can see the percentage of disc perforation and normal appearance.
Subjective Assessment of Triangular Fibrocartilage Complex Tears
The patient will usually report ulnar-sided wrist pain, which will often occur with popping or clicking. The mechanism of injury will suggest either repeated forceful twisting or pulling movements, or a fall/traumatic incident. The mechanism will direct you to either an acute/traumatic injury considered to be type 1 TFCC injures, or a degenerative/repetitive injury which are type 2 injuries. The symptoms will be mechanical in nature – improving with rest and worsen with activity.
Examples of mechanisms:
- Wrist related activities common to the sports listed above
- Falling onto a pronated and extended wrist
- Strong distraction force applied to the wrist/forearm
- Power-drill injuries in which the drill binds and rotates the wrist instead of the bit
- Distal radius fractures (possible as the result of a mechanism listed above or other)
Patients will be at an increased risk of degenerative TFCC tears if they have a previous history of wrist trauma or a congenital abnormality causing the ulnar to be longer than the radius (Markolf, Lamey, Yang, Meals, & Hotchkiss, 1998).
They will report decreased grasp strength, and limitations with work or sporting activities. Activities they could report as causing pain include turning a door handle, lifting heavy objects, pushing themself up from a chair. They may also report crepitus, instability, catching or swelling.
For a more detailed classification of TFCC injuries look here.
Physical Examination of Triangular Fibrocartilage Complex Tears
As mentioned before, there are many different causes of wrist pain – this article is just looking at TFCC injuries and as such will we not be discussing every appropriate wrist test for a complete differential diagnosis. However, you should ensure that you complete a thorough examination.
Some of the general examination findings common to TFCC injuries include;
- pain on resisted wrist ulnar deviation and dorsiflexion
- a clicking sensation on wrist movement
- reduced grip strength
- tenderness and swelling over the dorsal ulnar aspect
- signs of trauma (bruising, abrasions)
Special Tests for Triangular Fibrocartilage Complex Tears
There are several tests for the wrist; these tests will help with the differential diagnosis of wrist pain. For this article we will just focus on a number of the tests that look specifically at TFCC injuries.
NB: Click each image below to enlarge.
Piano Key Sign Test
Press Test
Ulnomeniscal Triquetral Dorsal Glide Test
Ulnar Fovea Test
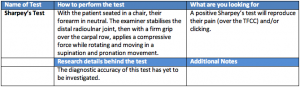
Sharpey’s Test
It should be remembered that the ‘gold standard’ is still considered to be an arthroscopic procedure (Prosser, Harvey, LaStayo, Hargreaves, Scougall, & Herbert, 2011).
A Very Unstable TFCC Joint
Imaging Assessment of Triangular Fibrocartilage Complex Tears
X-rays
A simple imaging option is x-rays. As with many conditions treated by physiotherapists the key structure, the TFCC, cannot be seen on a plain x-ray. However, an x-ray can offer some additional information. A PA x-ray of the wrist in neutral rotation can be used to assess for ulnar/radial variance, a positive (ulna longer) variance has been associated with TFCC injuries (Buterbaugh, Brown, & Horn, 1998). The x-ray can also be used to rule out associated fractures or dislocations with traumatic injuries.
Due to low specificity wrist arthograms are considered of poor diagnostic significance.
MRI
High quality MRI’s can show the TFCC. The exact sensitivity and specificity will vary across the different possible locations of damage (Tanaka, Yoshioka, Ueno, Shindo, & Ochiai, 2006). However, the estimated sensitivity and specificity of MR images are 60% and 90% respectively (Brukner & Khan, 2011). This suggests that while a negative MRI finding does not necessarily rule out a TFCC injury, a positive MRI finding is strongly suggestive of an injury to the TFCC. Fat suppressed MRI scans are considered the best to exhibit the TFCC.
Conservative Physiotherapy Management of Triangular Fibrocartilage Complex Tears
As with many injuries you see, the best treatment option will require significant deliberation and input from treating practitioners and patient alike. TFCC injuries can occur as an acute (traumatic) injury or a degenerative injury; because of this the best approach to each injury will vary.
Some of the other factors that may alter your treatment are;
- severity of the injury (anatomically – what structures are involved),
- degree of functional impairment (including pain, irritability, ROM, etc.),
- ‘social’ factors (family, work and sporting commitments)
Type One Triangular Fibrocartilage Complex Tears (Traumatic)
As with many conditions it is preferential to manage a type one TFCC tear conservatively. The principles of the management follow a familiar pattern – reduce pain/swelling, restore movement, restore/rehab strength and function. The phases are not distinct; the management therefore has to overlap accordingly to ensure efficiency. However, for convenience I will break the phases up for the purposes of this article. Please note that no data was found regarding conservative management outcomes.
Reduce Pain/Swelling
After taking the irritability of the pain into consideration a course of action must be determined. The initial steps will be to rest the injured wrist, with this consider the relative rest approach. While it is vital to avoid any aggravating activities it is important not to allow any excessive function loss during this time. Ice can be used to help manage both the pain and swelling. Depending on the irritability, a period of immobilisation may be required. Typically three to six weeks duration is recommended. Splinting duration should be kept to a minimum where possible to reduce the negative secondary effects. If splinting will be required it is essential that the physiotherapist advises the patient to keep the uninvolved joints active. This will include regular exercises for the fingers/thumb, elbow, shoulder and neck. A course of NSAIDs may be discussed with the appropriate health practitioner. The duration of relative rest/immobilisation can be used to educate the patient, things that should be discussed would include:
- What to expect after the period of immobilisation (atrophy, reduced ROM, etc.)
- The importance to complete the appropriate exercises
- The cause of the injury, and if applicable, ways to avoid re-injury in the future
- The return to work/sport process
This approach may differ depending on the demands on the patient; elite athletes may only give conservative management two to three weeks before opting to undergo a wrist arthroscopy (Parmelee-Peters & Eathorne, 2005).
Key Components:
- Relative rest/Immobilisation
- Ice
- NSAIDs
- Maintenance exercises
- Education
Restore Movement
Now it is time for the physiotherapists to pull up their sleeves and make use of their great hands on abilities. A range of techniques can be used to enhance the patient’s response to this phase. I doubt any of these will be new so I’ll just list them;
- Soft tissue techniques – Massage, trigger point work, myofascial release
- Thermotherapy
- Passive movements, mobilisations and glides
- Stretches
- Exercises (both active and assisted active range of movement) targeting the involved joints
- Wrist (flexion/extension/ulnar deviation/radial deviation/pronation/supination)
- Fingers/Thumb (flexion/extension/opposition/grip)
- Elbow (flexion/extension)
- Shoulder/neck exercise can continue depending on the impairments found, it is important to have a strong base for upper limb movements
During this phase a removable splint may also be used to provide additional protection. If required the splint can be worn during the night or at work/during modified training sessions.
Key Components:
- Manual techniques
- ROM exercises
- Education
Restore Strength and Function
As the movement returns the exercises can be progressed into strengthening exercises, progressively increasing the load. The exercises should not aggravate any symptoms. All of the exercises listed above can be used to direct what strengthening exercises will be needed.
Due to the variety of situations the more specific work/sport return to function process is beyond the scope of the article. You will have to draw on your experience and work with the appropriate coaches/return to work coordinators to ensure the appropriate outcomes are achieved prior to returning to full duties at work or a competitive level in sport.
Key Components:
- Progressive strengthening exercises
- Functional activity specific exercises
- Education
Type Two Triangular Fibrocartilage Complex Tears
A degenerative TFCC that has become painful raises two questions in my mind. The first being, what has caused the pain, has the TFCC finally sustained too much damage from the ‘wear and tear’ process or is the pain actually from a one off incident where the structure was over-loaded. Think chronic verse acute on chronic. In the case of the acute overload the conservative management approach detailed above should be considered. A patient with a symptomatic degenerative TFCC may need to consider surgery, this would be due to the poor healing capabilities of the central 80% the TFCC. The surgery would be aimed at tightening the supporting ligaments and shorten the ulna (where appropriate).
Surgical Management of Triangular Fibrocartilage Complex Tears
If surgery is undertaken the rehabilitation will follow the protocol as advised by the surgeon. It will vary depending on what was found during the procedure, if other structures were involved this will likely change the expected recovery time. As a guide if only the TFCC is involved the surgeon will place sutures and debride as required. In the sporting population following this operation the patient should be aiming for full return to sport after four to eight weeks of rehabilitation, depending on the sport. The primary indication for surgery was a lack of response to conservative treatment (Lubiatowski, Romanowski, Splawski, Manikowski, & Orgodowicz, 2006).
The outcomes from surgery depend on the classification of the injury, as this will change what is done during surgery. The method of surgery should be discussed with the surgeon, and they will also be able to give a better idea of prognosis. In general, arthroscopic repair of a TFCC tear achieves “good to excellent” results in 63% of cases (Reiter, et al., 2008). Below is a table to give a summary of the expected outcomes based on the injury type.
Examples of Appropriate Outcome Measures
- Grip strength (can be measured with a Jamar dynamometer)
- For normative data on grip strength download this PDF
- Range of motion of wrist
- A quick reference for some normative values of wrist ROM
- Patient Rated Wrist Evaluation
- For the APA appraisal download this PDF
- Patient specific outcomes
Clinical Implications and Take Home Messages
- The anatomy around the wrist is complex, detailed knowledge is vital to provide accurate information for your patients.
- TFCC injury mechanisms will often involve repetitive high forces on the wrist, extension and/or ulnar deviation and often caused during weight bearing load or from a fall.
- TFCC injuries are considered in two types. Type one injuries are acute injuries to the TFCC, whereas the type two injuries are degenerative injuries.
- There are many different tests for the wrist, better knowledge of the anatomy of the region and good palpation skills will guide you to which wrist tests to use. Be aware of the specificity and sensitivity of the different tests so help you weigh the influence of their outcomes on your diagnosis.
- TFCC injuries can often be managed conservatively, however failing this or under some circumstances surgery should be considered as an option. There is a need for more research to better direct treatment.
What Are Your Thoughts?
Do you have any interesting experiences with TFCC tears that you would like to share? Because I would love to hear about them and your thoughts on the matter! Leave a comment below or catch me on Facebook or Twitter.
Are you a physiotherapist or physical therapist looking to promote your own clinic, check this out.
About The Author
This is another guest post from Christopher Snell. Christopher is an Australian physiotherapist who graduated from Monash University (Melbourne). Professionally he has worked with local level swimming and football (both soccer and AFL) clubs as a sports trainer, strength and conditioning coach and physiotherapist. His clinical interests include acute sports injuries, knee rehabilitation and dry needling. He is currently employed at Waverley Park Physiotherapy Centre.
Photo Credit: World Series Boxing
References
Brukner, P., & Khan, K. (2011). Clinical Sports Medicine (4th ed.). Sydney: McGraw-Hill Australia Pty Ltd.
Buterbaugh, G., Brown, T., & Horn, P. (1998). Ulnar-sided wrist pain in athletes. Clinical Sports Medicine, 17(3), 567-583.
de Araujo, W., Poehling , G., & Kuzma , G. (1996). New Tuohy needle technique for triangular fibrocartilage complex repair: preliminary studies. Arthroscopy, 12(6), 699-703.
LaStayo, P., & Howell, J. (1995). Clinical Provocative Tests Used in Evaluating Wrist Pain:A Descriptive Study. Journal of Hand Therapy, 8(10), 10-17.
Lester, B., Halbrecht, J., Levy, M., & Gaudinez, R. (1995). “Press Test” for Office Diagnosis of Triangular Fibrocartilage Complex Tears of the Wrist. Ann Plast Surg, 35, 41-45.
Lindau, T., Adlercreutz, C., & Aspenberg, P. (2000). Peripheral tears of the triangular fibrocartilage complex cause distal radioulnar joint instability after distal radial fractures. Journal of Hand Surgery, 464 – 468.
Lubiatowski, P., Romanowski, L., Splawski, R., Manikowski, W., & Orgodowicz, P. (2006, June). Treatment of injury of the triangular fibrocartilage complex. Ortop Traumatol Rehabil, 8(3), 256-262.
Markolf, K., Lamey, D., Yang, S., Meals, R., & Hotchkiss, R. (1998). Radioulnar Load-Sharing in the Forearm. The Journal of Bone and Joint Surgery, 879-888.
Mikic, Z. D. (1978, June). Age changes in the triangular fibrocartilage of the wrist joint. Journal of Anatomy, II(126), 367-384.
Minami, A., & Kato, H. (1998). Ulnar shortening for triangular fibrocartilage complex tears associated with ulnar positive variance. J Hand Surg Am, 23(5), 904-908.
Nakamura, T., Yabe, Y., & Horiuchi, Y. (1996). Functional Anatomy of the Triangular Fibrocartilage Complex. Journal of hand Surgery British and European, 581-586.
Palmer, A. K., & Werner, F. W. (1981). The triangular fibrocartilage complex of the wrist anatomy and function. Journal of Hand Surgery America, 6(2), 153-162.
Parmelee-Peters, K., & Eathorne, S. (2005). The Wrist: Common Injuries and Management. Primary Care: Clinics in Office Practice, 35-70.
Prosser, R., Harvey, L., LaStayo, P., Hargreaves, I., Scougall, P., & Herbert, R. D. (2011). Provocative wrist tests and MRI are of limited diagnostic value for suspected wrist ligament injuries: a cross-sectional study. Journal of Physiotherapy, 57, 247-253.
Reiter, A., Wolf, M. B., Schmid, U., Frigge, A., Dreyhaupt, J., Hahn, P., et al. (2008, November). Arthroscopic Repair of Palmer 1B Triangular Fibrocartilage Complex Tears. Arthroscopy: The Journal of Arthroscopic and Related Surgery, 24(11), 1244-1250.
Sagerman , S., & Short, W. (1996). Arthroscopic repair of radial-sided triangular fibrocartilage complex tears. Arthroscopy, 12(3), 339-342.
Tanaka, T., Yoshioka, H., Ueno, T., Shindo, M., & Ochiai, N. (2006, October). Comparison between high-resolution MRI with a microscopy coil and arthroscopy in triangular fibrocartilage complex injury. Journal of Hand Surgery America, 31(8), 1308-1314.
Tay, S. C., Tomita, K., & Berger, R. A. (2007). The “Ulnar Fovea Sign” for Defining Ulnar Wrist Pain: An Analysis of Sensitivity and Specificity.
Trumble, T., Gilbert, M., & Vedder, N. (1997, January). Isolated tears of the triangular fibrocartilage: management by early arthroscopic repair. J Hand Surg Am, 22(1), 57-65.
Related Posts
Comments
Trackbacks
-
[…] Meet – Chris Bartl Posture Part 3: Optimizing Sitting – The Manual Therapist Triangular Fibrocartilage Complex Tears – The Sports Physiotherapist Train Heavy Loads to Burn More Energy and Lose Fat -Charles Poliquin Step Your Game Intelligence Up […]














Very informative! I was advised to read this by my osteopath as we suspect that I may have a TFCC problem. From reading this I think we are right and it is a type 2 tear I’m a competitive strongwoman and powerlifter and really don’t want to have surgery, at the moment I can train most movements as ling ad I heavily strap my wrist up and I use Ibuprofen gel and freeze spray when competing as well as strapping. Not sure what else to do really?
I’m a competitive strongwoman and powerlifter and really don’t want to have surgery, at the moment I can train most movements as ling ad I heavily strap my wrist up and I use Ibuprofen gel and freeze spray when competing as well as strapping. Not sure what else to do really?