Introduction
Groin pain is a common complaint in sports involving running, kicking and explosive changes of direction, and as such is frequently encountered by the sports physiotherapist. In soccer, groin and lower abdominal pain accounts for 10-13% of injuries per year (1). However, due to the number of potential differential diagnoses for athletes with chronic pain in the groin and lower abdominal region only a small proportion of athletes are eventually diagnosed with athletic pubalgia (sports hernias).
Athletic pubalgia is a poorly understood disease process and may also be known as sports hernias, Gilmore’s groin, pubic inguinal pain syndrome or sportsmen’s groin. Though many cases of groin/abdominal pain are self-limiting and only a minority of cases are symptomatic for more than three weeks, it is imperative that athletes with the condition are managed appropriately as the symptoms can eventually limit the athlete’s participation in training and playing.
Pathogenesis of Athletic Pubalgia
Currently there are two schools of thought that are emerging with regards to the pathogenesis of athletic pubalgia.
- One theory is characterised by muscular injury and disruption:
- Gilmore (2) found that athletes presented with:
- A torn external oblique aponeurosis causing dilation of the superficial inguinal ring
- A torn conjoined tendon
- Dehiscence between the inguinal ligament and the torn conjoined tendon
- Tayler et al (3) suggested that athletes may be diagnosed with pubalgia “if physical examination does not reveal an inguinal hernia and there is an absence of other etiology for lower abdomen and groin pain”.
- Meyers et al (4) characterised the injury further as a hyperextension injury where the pubis acts as a pivot point into which rectus abdominis and adductor longus insert. Thus causing each muscle to pull against each other and cause injury (generally to the weaker abdominal wall muscle). Credence is lent to this suggestion by the high prevalence of concomitant adductor symptoms.
- Gilmore (2) found that athletes presented with:
- The second theory focuses on the concept of athletic pubalgia as a deficit in the transversalis fascia, which forms the posterior wall of the inguinal canal (5).
- Polglase et al (6) concluded from their study that the most common finding in athletes with chronic lower abdominal and groin pain was a deficiency of the posterior wall of the inguinal canal.
Despite the differing theories regarding the causes of athletic pubalgia, studies have found that subjects can present with both abnormalities in the posterior wall of the inguinal canal, the conjoined tendon/abdominal musculature. Therefore suggesting that both theories may in fact be linked.
Differential Diagnoses for Groin Pain
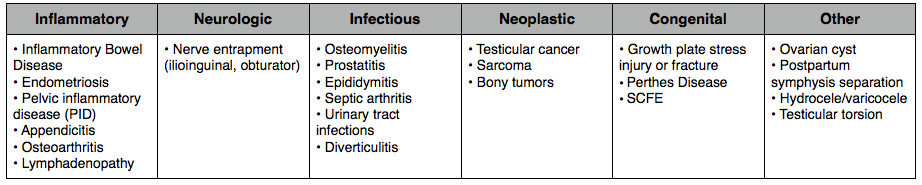
When it comes to groin pain, as we all know, there are so many differential diagnoses. Below there is a list of some musculoskeletal differential diagnoses (8, 9) that should be considered. These include:
- Stress fracture
- Muscle strain
- Muscle contusion or haematoma
- Tendon rupture (adductors)
- Adductor tendinopathy
- Bursitis
- AVN of the femoral head
- Labral tears
- Osteitis Pubis
- Femoroacetabular Impingement
- Pubic instability
- Lumbar Spine referral
- Sacroiliac joint referral
- Inguinal/femoral hernia
- Hip flexor/iliopsoas injury (tendinosis)
- Iliac apophysis injury
- Symphyseal instability
- Hip osteoarthritis
It is also worth noting that there are potential non-musculoskeletal causes of groin pain (8,9). Below is a table of a few that you should be mindful of.
Clinical Presentation of Athletic Pubalgia
The athlete with athletic pubalgia will often report:
- Pain: exercise related lower abdominal and groin pain that can radiate to the perineum, inner thigh and scrotum.
- Pain Quality: often the pain is described as deep and intense and is usually unilateral.
- Mechanism: symptoms are usually insidious in onset but occasionally athletes report a specific event that leads to injury.
- Population: generally athletes that present with the condition participate in high level sport and are involved with high intensity training, but will often not present for treatment until their symptoms have been present for a few months as athletes can often continue to play despite the pain.
- Aggravating Factors: sudden acceleration, twisting turning, cutting, kicking, sit ups, coughing/sneezing
- Easing Factors: rest
Physical Examination of Athletic Pubalgia
- There may be localised tenderness on or above the pubic tubercle on the affected side, inguinal canal tenderness, dilated superficial inguinal ring, and tenderness at the hip adductor origin
- Pain on resisted sit-up
- There is tenderness on or near the rectus insertion, lateral edge of rectus or the conjoined tendon/rectus abdominis interface
- There will be no bulge or cough impulse at the external inguinal ring, as this may indicate an inguinal hernia.
- No dilation of the external ring
Imaging for Athletic Pubalgia
The most important diagnostic tool in the assessment of an athlete with chronic abdominal and groin pain is the history and physical examination. However, there are several imaging options available to assist or confirm a clinical diagnosis:
- Plain radiograph or computed tomography may be useful in ruling out bony pathologies as the cause of the symptoms.
- Dynamic ultrasound may have a role in establishing posterior inguinal wall deficiencies.
- MRI is essential to assess the entire region and may identify conditions affecting the joints and soft tissues. Zoga et al (7) found that MR imaging is both sensitive (98%) and specific (89%–100%) in patients with athletic pubalgia for injuries involving the rectus abdominis, the adductor tendon origin, and the symphysis itself.
Interestingly, Letwin et al (1) suggest that herniography does not have a role in the diagnosis of athletic pubalgia as it is an invasive investigation that has a high complication rate.
Conservative Physiotherapy Management of Athletic Pubalgia
Unfortunately for the athlete with athletic pubalgia, conservative management is unlikely to resolve their symptoms and they are likely to require surgery (1). However, for the ‘in-season’ athlete who cannot afford to take time off for surgery, they may attempt a four week trial of “rest” where the player participates in a programme of closed-chain lower extremity exercises, selective steroid or platelet rich plasma injections to the rectus abdominus insertion/adductor longus origin. These measures may reduce acute symptoms to facilitate a return to play, but they are likely to be palliative only.
Should the athlete continue to be symptomatic at this stage, which is common for this condition, they may choose to return to sport regardless and undergo a surgical intervention once their competitive season is complete. Thankfully it is not thought that continued activity is likely to worsen the tear or results of a subsequent surgical repair.
Surgical Management of Athletic Pubalgia
Although there are many surgical interventions available, they tend to fall into three main categories:
- Laproscopic Mesh Placement – including Transabdominal Preperitoneal (TAPP) Hernia Repair and Totally Extraperitoneal (TEP) Hernia Repair
- Open Sutures Repair
- Open Mesh Repair
Debate persists on the density, specifically the weight and porosity of the mesh used as it may influence the amount of scarring, flexibility, whether the mesh is palpable, the presence of chronic pain and hernia reoccurrence. Sutured repairs are often preferred in the athletic population as they allow the surgeon to reinforce the posterior inguinal wall and create stability at the pelvis by broadening the rectus abdominus insertion. However, athletes may find that the tension caused by the sutures can cause more pain post-op so additional analgesia may be required.
Great Video Explanation
Post-Operative Rehabilitation for Athletic Pubalgia
As you may expect, the post-operative rehabilitation will vary dependent upon the preference of the orthopaedic surgeon and the surgery performed. However, this is a general overview of rehabilitation. Usually the surgery is performed as an outpatient procedure, and athletes are allowed to weight bear as tolerated afterwards. A period of relative rest is advised for the first ten days, particularly until the wound is checked. The athlete will then progress through a programme of hip range of motion exercises, closed chain lower limb exercises, core strengthening exercises (at four weeks) and sports specific drills are introduced at about week five. Normally a full return to sport is anticipated at approximately six weeks post-op.
Take Home Messages
- Athletic pubalgia is a distinct syndrome of lower abdominal/groin pain found in high performance athletes
- The symptoms are likely caused by muscle injury that may lead to further injury of the transversalis fascia
- Athletic pubalgia should be on your list of differential diagnoses of athletes presenting with groin pain, particularly chronic pain that has not responded to conservative management
- These athletes will often require a surgical repair
- The principles of surgical repairs involve:
- Fixation of rectus abdominis
- Reinforcement of the posterior wall of the inguinal canal
What Are Your Thoughts?
Do you have experience treating or assessing athlete’s suffering from athletic pubalgia/sports hernia. If so, I would love to hear your thoughts and experiences, so be sure to let me know in the comments or catch me on Facebook or Twitter.
Are you a physiotherapist or physical therapist looking to promote your own clinic, check this out.
About the Author
This was another great guest post by UK Physiotherapist Laura Chimimba. Laura graduated from Glasgow Caledonian University in 2006, and since graduation has had the opportunity to work at various levels of football. She has been involved with the treatment and rehabilitation of players from amateur, professional youth academy and elite level women/girls players. She is currently the Head Physiotherapist at Stenhousemuir FC. In addition to her sports coverage, Laura also works within the NHS and in private practice at Move Well Physiotherapy near Falkirk. This allows her to work closely with a variety of Orthopaedic and Sports Medicine Specialists. Furthermore, Laura has continued to further her education and has recently began a MSc in Sport and Exercise Medicine. Fortunately for her patients, and you as the reader, she continually strives to enhance her clinical skills and stay up to date with current evidence based practice.
References
(1) Litwin D, Sneider, E.B, McEnaney, P.M & Busconi, B.D (2011) Athletic pubalgia (Sports Hernia), Clinics in Sports Medicine, Vol 20(2), pp417-434
(2) Gilmore, O.J (1991) Gilmore’s groin: ten years experience of groin disruption – a previously unsolved problem in sportsmen, Sports Med Soft Tissue Trauma, Vol 1(3), pp12-14
(3) Taylor, D.C, Meyers, W.C, Moylan, J.A, Lohnes, J, Bassett, J.H & Garrett, W.E (1991) Abdominal musculature abnormalities as a cause of groin pain in athletes: inguinal hernias and pubalgia, American Journal of Sports Medicine, Vol 19(3), pp239-242
(4) Meyers, W.C, Foley, D.P, Garrett, W.E, Lohnes, J.H & Mandlebaum, B.R (2000) Management of severe lower abdominal or inguinal pain in high-performance athletes, American Journal of Sports Medicine, Vol 28, pp2-8
(5) Malycha, P & Lovell, G (1992) Inguinal surgery in athletes with chronic groin pain: the ‘sportsman’s’ hernia, Australian and New Zealand Journal of Surgery, Vol 62, pp 123-125
(6) Polglase, A.L, Frydman, G.M & Farmer, K.C (1991) Inguinal surgery for debilitating chronic groin pain in athletes, Medical Journal of Australia, Vol 155, pp674-677
(7) Zoga, A.C. Kavanagh, E.C., Omar, I.M., Morrison, W.B., Koulouris, G., Lopez, H., Chaabra, A., Domesek, J., Meyers, W.C. (2008) Athletic Pubalgia and the “Sports Hernia”: MR Imaging Findings, Radiology, 247, 797-807.
(8) LeBlanc, K.E., LeBlanc, K.A. Groin pain in athletes. Hernia 2003;7:68–71
(9) Caudill P, Nyland J, Smith C, et al. Sports hernias: a systematic literature review. Br J Sports Med 2008;42:954–64.
Photo Credit: LEIJONAT
Related Posts
Comments







what are your thoughts on the LLOYD release procedure and his theories of groin pain and management?
is it worth the surgery?