Introduction
Lateral epicondylalgia (tennis elbow) is a condition that I, and am sure many other physiotherapists out there, treat very commonly. This is not surpising given that it has an annual prevalence of 1% to 2% in the general public (Shiri et al., 2006). Furthermore, this condition is even more common in particular groups of athletes, as an example, it has been suggested that nearly 40% to 50% of recreational tennis players will suffer this condition during their lifetime (Hume et al., 2006; Mackay et al., 2003). Interestingly, despite the frequency with which healthcare is sought for this condition; only recently has our understanding of the pathophysiology of lateral elbow overuse injury improved. Consequently, the treatment approaches for lateral epicondylalgia vary widely and lack definitive evidence. Therefore, this article will discuss the evidence based assessment and management of lateral epicondylalgia (tennis elbow).
Pathoanatomy of Lateral Epicondylalgia
Lateral epicondylalgia was previously referred to as lateral epicondylitis or tendinitis. However, the terms epicondylitis and tendinitis are misleading because they suggest an inflammatory process. However, following histopathological studies we now know that the pathophysiology of this condition is degenerative in nature and that the injury occurs as a result of microtrauma (Kraushaar and Nirschl, 1999).
The pathological process has been termed angioblastic tendinosis (Kraushaar and Nirschl, 1999). As with many overuse tendon pathologies; fibroblastic and vascular degeneration occurs secondary to repetitive activities (typically rotation of the forearm and forceful gripping). Anatomically, the extensor carpi radialis brevis (ECRB) is the most commonly affected tendon, although other tendons in the extensor bundle, such as the extensor digitorum communis (involved in approximately 30% of cases), may be involved (Taylor & Hannafin, 2012).
It has been suggested that there are four stages of lateral epicondylalgia (Nirschl, 1988);
- Early Inflammatory Reaction
- Angiofibroblastic Degeneration
- Structural Failure
- Fibrosis or Calcification
Not surprisingly, this suggestion seems to follow the new continuum concept of tendinopathies (if you have not yet read this article, it is well worth checking out). This article will give you an insight into the underlying processes involved in tendinopathy, and its relevance to treatment decisions.
Subjective Assessment of Lateral Epicondylalgia (Tennis Elbow)
As per usual a comprehensive subjective examination should be performed and pertinent historical factors should be evaluated including hand dominance, load history, and previous episodes/treatments.
The patient/athlete with lateral epicondylalgia will often report:
- History: often results secondary to occupational/recreational/habitual overuse or as a result of change in loading patterns. This may need to be explored, as it is often not obvious to the patient.
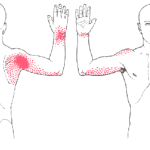
- Pain: ache pain and/or a burning sensation around the lateral humeral epicondyle and often down the forearm. Intermittent sharp pains may occur when performing aggravating activities.
- Aggravating Activities: generally those that require resisted wrist extension or gripping, e.g. pouring a jug, lifting weights.
- Easing Activities: frequently include rest, heat/ice and NSAIDs.
It is important that you try to establish the ‘stage’ (think of the continuum concept!) of lateral epicondylalgia, which will give you an idea of the quality of tendon tissue and the pathological processes that are occuring.
Objective Assessment of Lateral Epicondylalgia (Tennis Elbow)
The objective examination of patients with lateral epicondylalgia (tennis elbow) will likely show:
- Palpation: Tenderness to palpation at the lateral epicondyle and along the common extensor tendon is a hallmark of lateral epicondylitis. Swelling and ecchymosis are not typically present, and grip strength is usually reduced Nirschl (1999).
- Grip Strength: Dorf (2007) compared grip strength with the elbow in varying positions of flexion in a cohort of 81 patients diagnosed with lateral epicondylalgia. With the elbow in extension, the affected side had 50% grip strength when compared to the unaffected side.
- Resisted Extension: will likely be weakened and painful.
- Neural Examination: should be performed. Useful to exclude cervical pathologies and other differential diagnoses. Frequently, radial nerve tension tests will be positive.
Differential Diagnoses
If uncertainty exists, imaging and diagnostic tests can be useful for exploring the potential for a differential diagnosis, including (but not exhaustively):
- Radiocapitellar Chondromalacia
- Posterolateral Elbow Instability
- Plica
- Loose Bodies
- Malignancy
- Cervical Radiculopathy (C6 or C7)
- Compression of the Posterior Interosseous Nerve at the Arcade of Frosche (supinator syndrome) (Bisset et al., 2005; Taylor & Hannafin, 2012)
Imaging Assessment
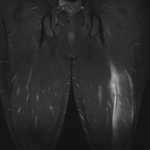
As suggested above, imaging is rarely required in lateral epicondylalgia as diagnosis is made clinically. However, magnetic resonance imaging (MRI) is helpful in evaluating the soft tissues of the elbow in patients who have failed appropriate conservative treatment. The results may be helpful in both confirmation of diagnosis and potential surgical planning.
Martin and Schweitzer (1998) reviewed the MRI findings from 24 patients with chronic lateral epicondylalgia (tennis elbow). They reported increased intra-tendon signal in 92% of patients (compared with 16% of controls). Other studies have shown thickening, bone marrow edema pattern, and tears of the common extensor tendon (Taylor & Hannafin, 2012).
Conservative Physiotherapy Management of Lateral Epicondylalgia (Tennis Elbow)
Fortunately, for us as physiotherapists and physical therapists, it has been suggested that non-operative management of lateral epicondylalgia will result in successful resolution of symptoms in 90% of patients (Hay et al., 1999). The following will discuss components of treatment for lateral epicondylalgia and the supporting/refuting evidence of each:
Activity Modification/Load Management: This is undoubtedly one of the most important aspects of treating athletes with this condition! However, because load management is hard to quantify it is something that is frequently glossed over within the research. Modifying or reducing the aggravating activities (within possible lifestyle/training limits) is not only a necessary component, but is absolutely essential to achieve the success of any treatment protocol. For many athletes this can seem like the end of the world, but through use of appropriate education and communication the athlete can be shown the necessity of such ‘relative rest’; especially given the overuse aetiology of lateral epicondylalgia.
Exercise: Pienimaki et al (1996) compared a six to eight week exercise programme of stretches and exercises (isometric and isotonic) with a treatment of pulsed US across the same time span. At the end of the program they showed that the standardised mean difference between the groups for pain (PVAS) at rest was 0.97 (95% CI 0.30 to 1.63) and 0.66 (95% CI 0.01 to 1.31) for PVAS under strain, in favour of the exercise group. In layman’s terms, this means that on average pain was rated about 1/10 better at rest in the exercise group when compared with the US group.
Progressive eccentric exercise has been shown to deliver superior results to non-strengthening control groups, with significantly greater reductions in pain and improvements in pain, function and tendon appearance on imaging (Croisier et al., 2007).
Manipulation Techniques: The studies included both local elbow and cervical spine techniques. In a meta-analysis Bisset et al. (2005) pooled the data evaluating elbow manipulation, which showed a positive immediate effect on measures of PFGS (SMD 1.28; 95% CI 0.84 to 1.73) and pressure pain threshold. To put this clinically, this equated to a difference of 43 N (4.38 Kg) for PFGS. Similarly, Vicenzino et al (1996) showed positive effects of a lateral glide of the cervical spine for PVAS and pressure pain threshold. However, a major deficit of the research is that it involved only a single treatment session and there were no long term follow up. In summary, there appears to be some evidence of positive initial effects in favour of elbow and cervical manipulative therapy techniques.
Taping and Orthotics: It has been suggested that bracing (forearm straps and cock-up wrist splints) can redirect the extensor force vector and may provide symptom relief. The systematic review by Bisset et al. (2005) suggested that further research is required before any firm conclusions can be draw on the impact of taping/orthotics for lateral epicondylalgia. Whilst Jensen et al (2001) found considerable improvements when they compared an off the shelf orthotic (Rehband) with a CSI over 6 weeks, Wuori et al (1998) showed no benefit of counterforce bracing over sham bracing.
With reference to taping, Vicenzino et al (2003) looked at the immediate effects of a diamond shaped taping technique and found a significant improvement in the intervention group for both PFGS (24% improvement from baseline) and pressure pain threshold immediately and 30 minutes after the intervention, when compared with a no intervention control. However, when compared with a placebo, there was no significant difference for measures of pain-free grip strength.
Acupuncture: There appears to be some evidence to support the efficacy of acupuncture over a placebo as a treatment for lateral epicondylalgia in short term outcomes. However, this benefit appears to be short lived—that is, two to eight weeks (Bisset et al., 2005)
Laser: six examined laser therapy; despite the presence of some contradiction in the short term effects of laser treatment, the pooled data presented show no evidence of effect over that of a placebo intervention, in either the short or long term.
ESWT: The pooled data from Bisset et al. (2005) included two studies which showed no significant treatment effect on pain (PVAS) or global improvement four to six weeks after treatment. This indicates that there was no added benefit of ESWT over that of placebo in the treatment of lateral epicondylalgia.
Combined Physical Interventions: Smidt et al (2002) evaluated a six week combined programme of massage, US, and exercises, and compared this group with a corticosteroid injection group and a wait and see (control) group. Over the long term (more than six months) results were favourable for the use a combined physical intervention approach when compared with a corticosteroid injection, however there was no significant difference to a wait and see (no treatment) approach.
Injection for Lateral Epicondylalgia (Tennis Elbow)
Corticosteroid Injections: The evidence supports short term benefit of corticosteroid injections only. Bisset et al. (2006) showed that corticosteroid injection showed significantly better effects at six weeks, however, there was a high recurrence rate. In fact 47/65 of successes subsequently regressed at 52 weeks and had significantly poorer outcomes in the long term compared with the physiotherapy group.
Prolotherapy: There are 2 RCT’s (Scarpone et al., 2005; Glick, 2006) and one prospective case series (Lyftogt, 2007) which evaluated the use of prolotherapy for lateral epicondylalgia. They displayed positive results, with improvements between 66% and 94% at up to 16 weeks.
Polidocanol: This is a vascular sclerosant, which is used to sclerose areas of high intratendinous blood flow, or ‘‘neovessels’’. Such “neovessels” are seen histopathologically in patients with lateral epicondylalgia. In a double-blind RCT, Zeisig et al (2008) compared the use of polidocanol with vasoconstrictive lidocaine/adrenaline injections. Interestingly, both groups improved their VAS pain scores at 3 months, without significant differences.
However, those patients who weren’t satisfied at three months follow-up were offered an additional injection session with polidocanol. Interestingly, at a 12 month follow-up those that received the additional polidocanol injections improved VAS scores by 51% (polidocanol) and 47% (lidocaine/adrenaline) compared with baseline.
Autologous Whole Blood: Three prospective case series assessing autologous whole blood were identified. Each study reported significant improvement compared with baseline: Edwards et al. (2003) reported 88%, Gani et al. (2007) reported 64%, and Connell et al. (2006) reported a median score of 0!
Platelet-rich Plasma (PRP): has been shown to effectively reduce pain and symptoms (Taylor & Hannafin, 2012). In a double-blind RCT, Gosens et al. (2011) displayed ongoing benefit of PRP injections (over corticosteroid injections) at a follow-up of 2 years. Interestingly, as suggested by the work of Bisset et al. (2006) those that underwent corticosteroid injections returned to baseline levels of pain and function over time.
Surgical Management of Lateral Epicondylalgia (Tennis Elbow)
In cases where nonoperative measures fail, surgery may be considered necessary. The surgical options for lateral epicondylalgia include:
- Percutaneous Techniques
- Open Techniques
- Arthroscopic Techniques
Surgical treatment involves release of the extensor tendon origin at the lateral epicondyle. Baker and Baker (2008) reported an 87% patient satisfaction rate in 42 patients treated arthroscopically at long-term follow-up (average of 10.1 years). Interestingly, Othman (2011) reported similar outcomes for arthroscopic and percutaneous techniques at 12 months’ follow-up. This percutaneous technique has been advocated as safe, reliable, and cost-effective (Taylor & Hannafin, 2012).
However, despite the generally positive results, there are inherent risks of surgery which include inadvertent neurovascular injury or release of the lateral ulnar collateral ligament (Kuklo et al., 1999; Smith et al., 2003).
Post-operative Rehabilitation
As is often the case, post-operative rehabilitation of surgical management of lateral epicondylalgia follows a sequential pattern. Whilst different surgeons and techniques will have varying post-operative protocols, there are generally 3 phases, including
- Protection of the Repair: frequently a cock-up wrist splint is used to protect the repair and to permit more active use of the elbow, whilst a sling is used for comfort. Range of motion of the elbow is instituted immediately.
- Stretching: The first 6 weeks following surgery are focused on recovery of range of motion of the wrist and elbow, which is performed as a home-based program including gentle stretching/ROM exercises.
- Strengthening: Formal physiotherapy/physical therapy is started at 6 weeks to restore full range of motion and restore full strength.
Clinical Implications and Take Home Messages
- Lateral epicondylalgia (tennis elbow) is a very common condition; in both athletes and the general public
- Pathology seems to follow the ‘continuum concept of tendinopathy’
- There are subjective and objective hallmarks of the condition
- Imaging is rarely required
- Conservative treatment is successful in 90% of cases
- There is no evidence for laser or ESWT
- There is some evidence of positive effects of exercise, manipulation/mobilisation, acupuncture, and combined interventions
- Injection therapies, other than corticosteroid injections, seem to show promising results
- Surgery is only required in recalcitrant cases, and shows favourable outcomes in this population
What Are Your Thoughts?
I am sure that you have experience assessing and rehabilitating athletes with this condition! What have you found useful and what treatments have you thrown away? I would love to know, so be sure to let me know in the comments (com’ on – help us all out!) or catch me on Facebook or Twitter.
Promote Your Clinic: Are you a physiotherapist or physical therapist looking to promote your own clinic, check this out.
References
Baker CL Jr, Baker CL 3rd. Long-term follow-up of arthroscopic treatment of lateral epicondylitis. Am J Sports Med. 2008;36(2):254-260.
Baumgard SH, Schwartz DR. Percutaneous release of the epicondylar muscles for humeral epicondylitis. Am J Sports Med. 1982;10(4):233-236.
Bisset L, Paungmali A, Vicenzino B, Beller E. A systematic review and meta-analysis of clinical trials on physical interventions for lateral epicondylalgia. Br J Sports Med 2005;39:411–422
Bisset L, Beller E, Jull G, Brooks P, Darnell R, Vicenzino B. Mobilisation with movement and exercise, corticosteroid injection, or wait and see for tennis elbow: randomised trial. BMJ: British Medical Journal. 2006;333(7575):939-941.
Bisson L, Moyer M, Lanighan K, Marzo J. Complications associated with repair of a distal biceps rupture using the modified two-incision technique. J Shoulder Elbow Surg. 2008;17(1):67S-71S.
Connell DA, Ali KE, Ahmad M, et al. Ultrasound-guided autologous blood injection for tennis elbow. Skeletal Radiol 2006;35:371–7.
Croiser JL, Foidart-Dessalle M, Tinant F, et al. An isokinetic eccentric program for the management of chronic lateral epicondylar tendinopathy. Br J Sports Med 2007;41:269–75.
Davidson J, Vandervoort A, Lessard L, et al. The effect of acupuncture versus ultrasound on pain level, grip strength and disability in individuals with lateral epicondylitis: a pilot study. Physiother Can 2001;53:195–202, 211.
Dorf ER, Chhabra AB, Golish SR, McGinty JL, Pannunzio ME. Effect of elbow position on grip strength in the evaluation of lateral epicondylitis. J Hand Surg Am. 2007;32(6):882-886.
Edwards SG, Calandruccio JH. Autologous blood injections for refractory lateral epicondylitis. J Hand Surgery Am 2003;28:272–8.
Fink M, Wolkenstein E, Luennemann M, et al. Chronic epicondylitis: effects of real and sham acupuncture treatment: a randomised controlled patient- and examiner-blinded long-term trial. Forsch Komplementarmed Klass Naturheilkd 2002;9:210–15.
Fink M, Wolkenstein E, Karst M, et al. Acupuncture in chronic epicondylitis: a randomized controlled trial. Rheumatology 2002;41:205–9
Gani NU, Butt MF, Dhar SA, et al. Autologous Blood Injection In The Treatment Of Refractory Tennis Elbow. The Internet Journal of Orthopedic Surgery 2007;5. http:// www.ispub.com/ostia/index.php?xmlFilePath=journals/ijos/vol5n1/tennis.xml
Glick RM. Prolotherapy for the treatment of lateral epicondylitis: A double-blind pilot study. North American Research Conference on Complementary and Integrative Medicine; 24–27 May 2006;
Edmonton, Canada.Gosens T, Peerbooms JC, van Laar W, den Oudsten BL. Ongoing positive effect of platelet-rich plasma versus corticosteroid injection in lateral epicondylitis: a double-blind randomized controlled trial with 2-year follow-up. Am J Sports Med. 2011;39(6):1200-1208.
Hay EM, Paterson SM, Lewis M, Hosie G, Croft P. Pragmatic randomised controlled trial of local corticosteroid injection and naproxen for treatment of lateral epicondylitis of elbow in primary care. BMJ. 1999;319(7215):964-968.
Hume PA, Reid D, Edwards T. Epicondylar injury in sport: epidemiology, type, mechanisms, assessment, management and prevention. Sports Med. 2006;36(2):151-170.
Jensen B, Bliddal H, Danneskiold-Samsoe B. Comparison of two different treatments of lateral humeral epicondylitis—‘‘tennis elbow’’. A randomized controlled trial (in Danish). Ugeskr Laeger 2001;163:1427–31.
Kraushaar BS, Nirschl RP. Tendinosis of the elbow (tennis elbow): clinical features and findings of histological, immunohistochemical, and electron microscopy studies. J Bone Joint Surg Am. 1999;81(2):259-278.
Kuklo TR, Taylor KF, Murphy KP, Islinger RB, Heekin RD, Baker CL Jr. Arthroscopic release for lateral epicondylitis: a cadaveric model. Arthroscopy. 1999;15(3):259-264
Lyftogt J. Subcutaneous prolotherapy treatment of refractory knee, shoulder and lateral elbow pain. Australasian Musculoskeletal Med 2007;12:110–12.
Mackay D, Rangan A, Hide G, Hughes T, Latimer J. The objective diagnosis of early tennis elbow by magnetic resonance imaging. Occup Med (Lond). 2003;53(5):309-312.
Martin CE, Schweitzer ME. MR imaging of epicondylitis. Skeletal Radiol. 1998;27(3):133-138.
Molsberger A, Hille E. The analgesic effect of acupuncture in chronic tennis elbow pain. Br J Rheumatol 1994;33:1162–5.
Nirschl RP. Prevention and treatment of elbow and shoulder injuries in the tennis player. Clin Sports Med. 1988;7(2):289-308.
Othman AM. Arthroscopic versus percutaneous release of common extensor origin for treatment of chronic tennis elbow. Arch Orthop Trauma Surg. 2011;131(3):383-388.
Pienimaki T, Tarvainen T, Siira P, et al. Progressive strengthening and stretching exercises and ultrasound for chronic lateral epicondylitis. Physiotherapy 1996;82:522.
Scarpone M, Rabago D, Zgierska A, et al. The efficacy of prolotherapy for lateral epicondylosis: a pilot study. Clin J Sports Med 2008;18:248–54.
Shiri R, Viikari-Juntura E, Varonen H, Heliovaara M. Prevalence and determinants of lateral and medial epicondylitis: a population study. Am J Epidemiol. 2006;164(11):1065-1074.
Smidt N, Van der Windt D, Assendelft W, et al. Corticosteroid injections, physiotherapy, or a wait-and-see policy for lateral epicondylitis: a randomised controlled trial. Lancet 2002;359:657–62.
Smith AM, Castle JA, Ruch DS. Arthroscopic resection of the common extensor origin: anatomic considerations. J Shoulder Elbow Surg. 2003;12(4):375-379
Stratford P, Levy D, Gauldie S, et al. The evaluation of phonophoresis and friction massage as treatments for extensor carpi radialis tendinitis: a randomized controlled trial. Physiother Can 1989;41:93–9.
Taylor SA, Hannafin JA. Evaluation and management of elbow tendinopathy. Sports Health: A Multidisciplinary Approach 2012;4: 384
Vicenzino B, Collins D, Wright. A. The initial effects of a cervical spine manipulative physiotherapy treatment on the pain and dysfunction of lateral epicondylalgia. Pain 1996;68:69–74.
Vicenzino B, Brooksbank J, Minto J, et al. Initial effects of elbow taping on pain-free grip strength and pressure pain threshold. J Orthop Sports Phys Ther 2003;33:400–7.
Wuori J, Overend T, Kramer J, et al. Strength and pain measures associated with lateral epicondylitis bracing. Arch Phys Med Rehabil 1998;79:832–7.
Zeisig E, Fahlstro¨m M, Ohberg L, Alfredson H. Pain relief after intratendinous injections in patients with Tennis elbow – results of a randomised study. Br J Sports Med 2008;42:267–71.
Image Credit: Dr Yuranga Weerakkody and Dr Bruno Di Muzio
Related Posts
Comments








In our schooling and research we’ve come across the use of eccentric exercises for lateral epicondylopathy (tennis elbow). Similar to the heel drop eccentric exercises for the achilles tendon, the exercise in this study showed significant improvements in the patient’s symptoms using eccentric exercises. What are your thoughts on the intervention?
http://www.ncbi.nlm.nih.gov/pubmed?term=Addition%20of%20isolated%20wrist%20extensor%20eccentric%20exercise%20to%20standard%20treatment%20for%20chronic%20lateral%20epicondylosis%3B%20a%20prospective%20randomized%20trial
Radio-Humeral MWM Lateral glides with the elbow in 10 degrees flexion and wrist 90 degrees pronation, while the patient is supine and grips a towel roll during the glide, which should be pain free or try medial MWM glides, whichever is painfree. Vary the angle until no pain is achieved with griping. You can use a hand-dynamometer as the outcome measure.
I find 3 sets of 5-10 twice weekly MWM with grip (depending when, if any pain sets in, otherwise use 10 if no pain is produced) followed by a progressive eccentric loading regimen for the wrist extenors starting with 1 lb-5lbs, a wrist flexor, pronator and supinaotr strengthening program progressing to a complete upper limb, elbow, shoulder and scapular stability program over approxiamately 5-6 weeks.
I also find taping effective, with one strip anchored on the lateral Humeral condyle pulling medially, proximally and just distal to the ECRB insertion and anchoring over the pronator teres. I get good results combining active release of the ECRB and L. Fascial rollers used manually also work wonders to release forearm extensor trigger points.
This works best with acute to subacute cases, with moderate benefit for chronic cases, which may take up to 12 weeks to resolve.
Billy Wavell BSc Sports and Exercise Science, Registered Physiotherapist
BC Canada
Thanks for the great info Billy – much appreciated!!