Introduction
Femoroacetabular impingement (FAI) is, as the name suggests, an impingement or abutment of the chondro-labral structures between the femur and acetabulum. Whilst the diagnosis of femoroacetabular impingement has only recently gained attention, it is known that the presentation is more common in the athletic population. High activity athletes are at increased risk; particularly athletes who participate in sports which require them to frequently move into a position of internal rotation and flexion. This makes it an important diagnosis for the sports physiotherapist to be aware of current research and the best practice.
Femoroacetabular Impingement: Cam, Pincer or Mixed
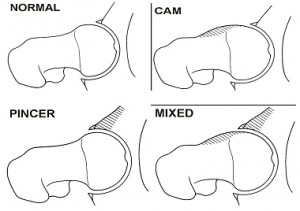
There are two subtypes of FAI; cam and pincer (Keogh et al 2008), which are discussed below:
CAM: Cam impingement occurs when the patient has an aspherical femoral head and there is an abnormal head/neck junction with an increased radius at the waist. At extremes of ROM this will result in femoral abutment causing sheer stress on the articular cartilage and a subsequent labral tear or detachment.
PINCER: Pincer impingement occurs when the patient has excessive acetabular coverage (or “over coverage”). This over coverage will cause femoral abutment against the chondrolabral tissues at extremes of ROM.
MIXED: The majority of cases are a mixed presentation of both
CAM and PINCER (Keogh et al 2008).
Assessment and Diagnosis of Femoroacetabular Impingement
The diagnosis of femoroacetabular impingement is made clinically and radiologically. The subjective, objective and imaging indicators are discussed below:
SUBJECTIVE: Clohisy et al. (2009) studied the clinical presentations of patients with symptomatic F.A.I. They found the athlete often presents with an insidious onset (65%) of groin (83%) or anterior hip pain. The pain is often intermittent, and exacerbated by physical activity (65%) and sitting (65%). A common misdiagnosis or competing hypothesis is a soft tissue injury of the groin or anterior hip musculature. This is an important differential diagnosis to be aware of.
OBJECTIVE: Phillipon et al (2006) found a significantly reduced range of motion in the symptomatic side of patients with FAI. They found differences in flexion (9 deg), internal rotation (4 deg), adduction (3 deg). The hip impingement test was positive in 99% of cases, and FABER’s in 97%.
These results are similar to those of Clohisy et al (2006). They found that the anterior impingement test reproduced anterior groin pain in 46 of 52 (88%) tested. 69% of patients had a positive FABER test, and 56% had a positive resisted straight leg raise.
IMAGING: Imaging can confirm the clinical diagnosis of FAI. Osseous abnormalities are identifiable on both X-ray and CT scanning, with increased accuracy achieved through CT. However, you should be aware of the increased radiation dosage associated with CT scanning. These will be useful in initial diagnosis to identify cam and pincer abnormalities.
MRI can be utilised articular cartilage and labral pathologies. Keeney et al (2004) evaluated the use of MR arthrography and showed limited sensitivity (47%) for articular cartilage pathology, but high specificity (89%). The high specificity makes a positive result more effective, resulting in a positive predictive value of 84% and an accuracy of 67% for cartilage damage.
For imaging the labrum MR arthrography seems to produce superior results. Byrd et al (2004) found a false negative of 42% with MR, however this was only 8% when using MR arthrograms for labral tears. The superiority of MRa is echoed by Czerny et al (1996) who showed a 91% accuracy for MR arthrography as opposed to 36% accuracy for MR alone.
Treatment for Femoroacetabular Impingement
CONSERVATIVE/PHYSIOTHERAPY MANAGEMENT: Unfortunately conservative physiotherapy management is often unsuccessful in young, highly activity athletes (Phillipon et al 2006). However, it may be helpful in some patients. The aims of physiotherapy are initially anti-inflammatory in nature. This includes rest from aggravating activities and electrophysical modalities. Other physiotherapy techniques you MAY find helpful in the early phases of treatment are:
- Pelvic/Gluteal Strengthening
- Core Stability Strengthening
- Gentle!!! Stretching
- Sometimes Mulligan (lateral hip distraction) techniques are useful (anecdotally)
SURGICAL MANAGEMENT: As previously stated, the majority of athletes will require surgery. Ng et al (2010) performed a systematic review on the efficacy of surgery for femoroacetabular impingement. They found that surgery was beneficial in the majority of presentations (~70%). They also showed that worse surgical outcomes were associated with increased levels of osteoarthritis, and these patients generally went on to to have a total hip replacement.
As for surgical options (which I know is not our decision to make), a systematic review by Bedi et al (2008) compared the outcomes of two surgical techniques; open and arthroscopic treatment of labral tears and FAI. They found insufficient evidence to support open surgical dislocation, the historic and supported gold standard, as a superior procedure to arthroscopic management.
RETURN TO PLAY OUTCOMES: Phillipon et al (2007) assessed the use of arthroscopic decompression in 45 professional athletes. The athletes, who were mostly male and hockey players, underwent surgery followed by an individualised (and poorly described) rehabilitation period. The athletes were allowed to return to play at 12 – 16 weeks post-operatively.
93% of the athletes returned to professional level sport. Supporting the findings of Ng et al (2010) the 3 athletes who did not RTP showed diffuse osteoarthritis on examination. Interestingly, 78% of athletes remained active in professional level sport at follow-up (an average of 1.6 years).
Clinical Implications
The real take home messages from this research is that:
- FAI should be considered as a cause of groin pain, particularly in an athletic population
- Early and correct clinical diagnosis is essential (remember to rule out competing hypotheses)
- Radiography should progress from initial Xray to MR arthrography to fully assess pathology
- The athlete should be educated on the usual clinical pathway of FAI (low response to conservative management)
- The athlete should undertake a short term conservative trial
- Surgical interventions should be considered early, given conservative treatment failure, as development of OA will decrease probability of successful outcome
- Arthroscopic decompression will allow the majority of professional athletes to return to play.
Man, what a long article. Hopefully you got something out of this. What are your thoughts or experiences dealing with femoroacetabular impingement? Be sure to let me know in the comments or catch me on Facebook or Twitter. Are you a physiotherapist or physical therapist looking to promote your own clinic, check this out.
If you require any sports physiotherapy products be sure check out PhysioSupplies (AUS) or MedEx Supply (Worldwide)
For more information check out these references!
References
Bedi A, Chen N, Robertson W, Kelly BT. The management of labral tears and femoroacetabular impingement of the hip in the young, active patient. Arthroscopy. 2008;24(10):1135-1145.
Byrd JWT, Jones KS. Diagnostic accuracy of clinical assessment, magnetic resonance imaging, magnetic resonance arthrography, and intra-articular injection in hip arthroscopy patients. Am J Sports Med 2004;32(7):1668–74.
Clohisy JC, Knaus ER, Hunt DM, Lesher JM, Harris-Hayes M, Prather H. Clinical Presentation of Patients with Symptomatic Anterior Hip Impingement. Clin Orthop Relat Res. 2009 March; 467(3): 638–644.
Czerny C, Hofmann S, Neuhold A, et al. Lesions of the acetabular labrum: accuracy of MR
imaging and MR arthrography in detection and staging. Radiology 1996;200:225–30.
Keeney JA, Peelle MW, Jackson J, et al. Magnetic resonance arthrography versus arthroscopy in the evaluation of articular hip pathology. Clin Orthop 2004;429:163–9.
Keogh MJ, Batts ME. A Review of Femoroacetabular Impingement in Athletes. Sports Med 2008; 38 (10): 863-878
Phillipon M, Schenker M, Briggs K, Kuppersmith D. Femoroacetabular impingement in 45 professional athletes: associated pathologies and return to sport following arthroscopic decompression. Knee Surg Sports Traumatol Arthrosc (2007) 15:908–914
Ng VY, Arora N, Best TM, Pan X and Ellis. TJ Efficacy of Surgery for Femoroacetabular Impingement : A Systematic Review Am J Sports Med 2010 38: 2337
Manaster BJ, Zakel S. Imaging of Femoral Acetabular Impingement Syndrome. Clin Sports Med 25 (2006) 635–657
Related Posts
In the past this site has featured some lighter, colloquial blog posts. These articles discuss issues related to the greater physiotherapy community. Thus, I present a few mantras I have heard, adapted or made up for the physios to live by in the coming year.
Radial tunnel syndrome is rare, it is challenging to differentially diagnose and can be a monster to manage. If you have a recalcitrant case of tennis elbow then this post will interest you! This article discusses the best available evidence for assessment and management of radial tunnel syndrome.